Khabor Wala Desk
Published: 4th February 2026, 3:18 AM
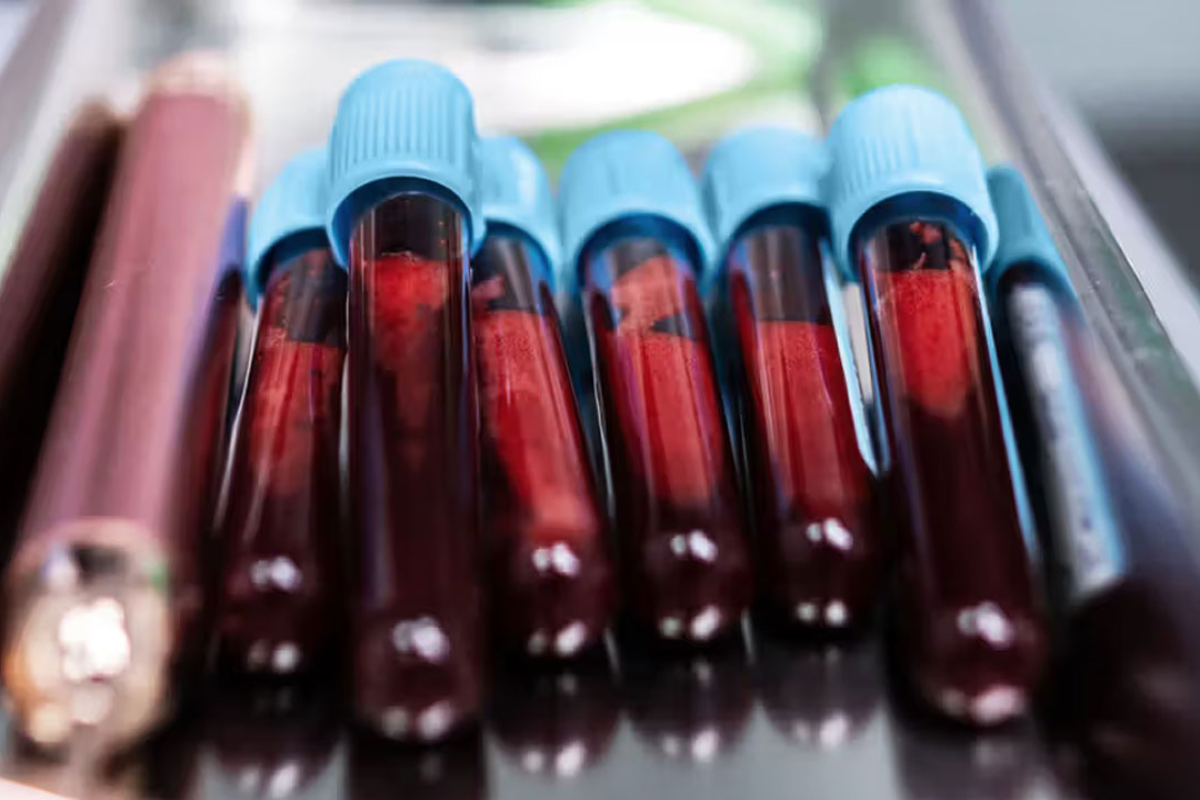
According to the World Health Organization (WHO), nearly 2.3 million women worldwide were diagnosed with breast cancer in 2022, making it one of the most prevalent malignancies affecting women globally.
Currently, breast cancer treatment involves a variety of approaches, including surgery, chemotherapy, radiotherapy, immunotherapy, and targeted therapies for specific cancer subtypes. However, not all treatments are equally effective for every patient. The success of therapy largely depends on factors such as the type and stage of cancer, as well as the patient’s overall health, making it challenging for clinicians to predict which treatment will yield the best outcomes for individual patients.
A recent study published in Clinical Cancer Research highlights a promising new diagnostic tool—liquid biopsy—that could transform treatment planning for advanced-stage breast cancer. This minimally invasive test measures circulating tumour DNA (ctDNA) in a patient’s blood, offering insights into how effectively a particular targeted therapy might work before treatment even begins.
In the study, researchers analysed blood samples from 176 patients participating in the PLASMA-MATCH trial. These patients had advanced breast cancer, some of whom had metastatic disease—cancer that had spread beyond the breast and lymph nodes to organs such as bones, liver, or lungs.
Participants were divided into two groups based on tumour genetics:
| Group | Genetic Characteristics | Number of Patients | Key Findings |
|---|---|---|---|
| Group 1 | ESR1, HER2, AKT1, AKT, or PTEN mutations | 88 | Patients with undetectable ctDNA at 4 weeks had progression-free survival (PFS) of 10.6 months; detectable ctDNA had PFS of 3.5 months. Treatment response: low ctDNA 46.2%, high ctDNA 7.9%. |
| Group 2 | Triple-negative, no detectable mutations | 88 | Low ctDNA at baseline: PFS 10.2 months, treatment response 40%; high ctDNA: PFS 4.4 months, response 9.7%. Patients with undetectable ctDNA after 4 weeks had PFS 12 months and 85.7% response; detectable ctDNA: PFS 4.3 months, 11.4% response. |
Researchers measured ctDNA levels before therapy and again four weeks into treatment. Findings showed that patients with low or undetectable ctDNA levels responded far better to therapy, while those with higher levels had significantly shorter progression-free survival and lower response rates.
Dr Isolt Brown, clinical research fellow at the Institute of Cancer Research, London, and lead author of the study, stated: “Analysing ctDNA from blood samples enables us to identify in advance which patients are likely to respond to therapy, providing a clearer roadmap for treatment planning.”
Dr Richard Reitherman, Medical Director at MemorialCare Breast Center, California, emphasised the significance for metastatic patients: “When cancer spreads to other organs, detection and effective treatment become far more complex. Liquid biopsy provides a rapid and accurate method to monitor response and adapt therapy accordingly.”
Dr Richard Zelkovits, Medical Director of Breast Oncology at Hartford Healthcare Cancer Institute, described the findings as “truly game-changing.” He explained that monitoring ctDNA allows clinicians to tailor therapies, improving patient outcomes and enabling timely adjustments in treatment.
This research demonstrates that liquid biopsy and ctDNA monitoring can provide critical, early insights into treatment efficacy, offering hope for patients with advanced and metastatic breast cancer. Beyond guiding therapy, it has the potential to improve survival rates and quality of life, marking a significant step forward in personalised cancer care.
Comments